No products in the cart.
A scan can feel like certainty. When pain lingers, movement is restricted and daily life starts to narrow, it is natural to want a picture of what is wrong. Many people assume an X-ray, CT or MRI is the quickest path to an answer. Sometimes it is. Quite often, it is not.
For common muscle, joint and back problems, the question is not whether scans are useful in medicine. They clearly are. The question is whether they are useful at this point, for this kind of pain, and whether the result will actually change what happens next.
That is where things become more nuanced. Across Australia and overseas, major clinical guidance is consistent on one point: routine imaging is not recommended for uncomplicated acute low back pain unless there are signs of a serious underlying cause. The reason is simple. In most cases, a scan does not improve outcomes, and it can complicate care by drawing attention to findings that are common in people with no pain at all.
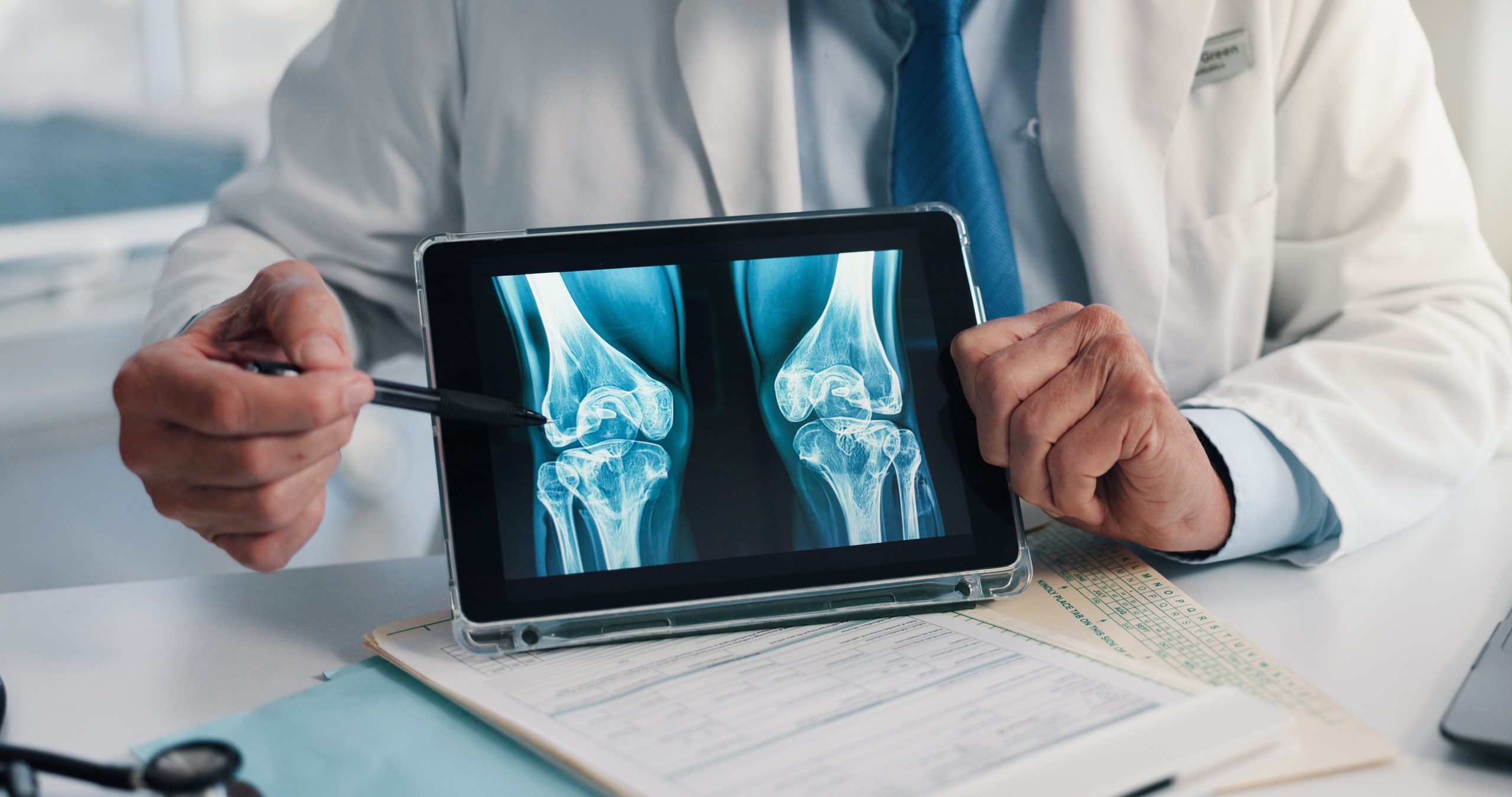
Why people want scans
This is easy to understand. Pain is unsettling, especially when it interrupts work, exercise or sleep. A scan promises clarity. It feels objective. It seems more convincing than being told to move, strengthen or wait and review.
But a scan is only useful if it answers the right question. A picture can show structures. It cannot, on its own, tell the whole story of why something hurts, whether that finding matters, or what the best next step should be.
When a scan really can help
There are times when imaging is important and should not be delayed. A scan may be appropriate when symptoms suggest a fracture, serious infection, inflammatory disease, cancer, or significant neurological compromise. Imaging can also be important after major trauma, or when symptoms are changing in a way that suggests something more than a straightforward musculoskeletal problem.
Some examples where urgent medical review may be needed include:
Those situations are not everyday aches and strains. They need careful screening and, in some cases, imaging sooner rather than later.
When a scan often does not change much
For many common presentations, especially recent low back pain without red flags, imaging does not improve recovery. That is because most acute episodes are not caused by something dangerous or surgically urgent. They are often related to joints, muscles, discs, soft tissues and movement patterns that respond to time, graded activity and targeted treatment.
Scans can also create a false sense of explanation. Words like “degeneration”, “bulge” and “wear and tear” can sound alarming, yet many of these findings are common in people who have no pain. Large reviews of spinal imaging have shown that disc degeneration, bulges and other changes become more common with age, even in people without symptoms.
That does not mean scans are useless. It means they need context.

The difference between seeing something and understanding it
A scan may show a disc bulge, but that does not prove the bulge is the reason for pain. It may show degenerative change, but that may simply reflect normal ageing. It may even look quite ordinary while a person is clearly in pain. This is where clinical assessment matters. How pain behaves often matters more than the image alone. Does it ease with gentle movement? Is it worse after prolonged sitting? Does it travel below the knee? Is there stiffness in the morning that settles, or pain that does not change no matter what position the person is in? Those patterns help determine whether physiotherapy is appropriate, whether review is needed, and whether imaging is likely to add useful information.
A clearer way to think about scans and pain
| Situation | A scan may be less useful | A scan may be more useful |
|---|---|---|
| Recent back pain with no red flags | Yes | No |
| Pain that changes with movement or position | Often | Sometimes |
| Pain after major trauma | No | Yes |
| Persistent pain with neurological changes | No | Yes |
| Pain that consistently disturbs sleep with other concerning symptoms | No | Yes |
| Established, uncomplicated flare-up that is improving | Often | Usually not |
This is not a substitute for clinical assessment. It is a way of showing that imaging is most useful when it changes management, not simply when pain is present.
Why unnecessary scans can make recovery harder
The risk is not only cost. Unnecessary imaging can increase worry, encourage over-medicalisation and pull attention away from the things that improve recovery, such as graded movement, strength, confidence and time. Guidance from Choosing Wisely Australia and the RACGP both note that scans can identify findings that are irrelevant to the current episode and can lead to further tests or procedures that do not improve outcomes.
This is especially important in back pain, where fear can become part of the problem. If a report sounds dramatic, people may start moving less, not more. That can shrink tolerance, reduce confidence and make recovery slower.
What people often need instead
For many musculoskeletal problems, the most useful early step is not imaging. It is a good assessment.
That usually includes:
This is often enough to decide whether the problem is likely to respond to hands-on treatment, exercise-based rehabilitation, watchful waiting, medical review, or imaging.
The aim is not to avoid scans at all costs
There are times when imaging is the right call. The point is not to be anti-scan. It is to use the right tool at the right time.
When a scan is clearly indicated, it can be valuable. It can clarify serious pathology, guide referral and inform treatment decisions. When it is used too early or for the wrong reason, it can create more confusion than clarity.
The most helpful question is not “Should I get a scan?” It is “Will a scan change what happens next?” That is where good clinical judgement makes all the difference.
When a scan is clearly indicated, it can be valuable. It can clarify serious pathology, guide referral and inform treatment decisions. When it is used too early or for the wrong reason, it can create more confusion than clarity.
The most helpful question is not “Should I get a scan?” It is “Will a scan change what happens next?” That is where good clinical judgement makes all the difference.
What does this mean in practice?
For many people with recent back, neck or joint pain, careful assessment and a clear plan are more useful than imaging in the first instance. For others, symptoms point to the need for further investigation and the scan becomes part of appropriate care.
The value of a scan is not in the image itself. It is in how well that image fits the person in front of it.
This article is general information only and does not replace individual medical advice. If you have unexplained pain, swelling, or neurological symptoms, consult a qualified healthcare professional before booking massage treatment.
