No products in the cart.
Pain during sex. Bladder leakage. A dull ache that never quite explains itself. For thousands of women, these symptoms have been tolerated, dismissed or treated as separate problems for years. There is a name for what connects them, and the treatment is often the opposite of what most people try first.
Somewhere in the vast cultural conversation about pelvic floors, a message has been repeated so often it has become automatic: strengthen. Squeeze. Do your Kegels.
The advice is everywhere, from postnatal pamphlets to wellness podcasts to well-meaning friends. And for a lot of people, it is exactly the right advice.
But for a significant number of women, strengthening is not only unhelpful. It can make things worse.
The reason is a condition that most people have never heard of: an overactive pelvic floor. The clinical term is hypertonic, and it describes pelvic floor muscles that are switched on too much of the time and struggle to relax when they are supposed to. Think of it as a fist that never fully opens. The muscles are not weak. They are exhausted from never letting go.
Why symptoms look like they have nothing in common
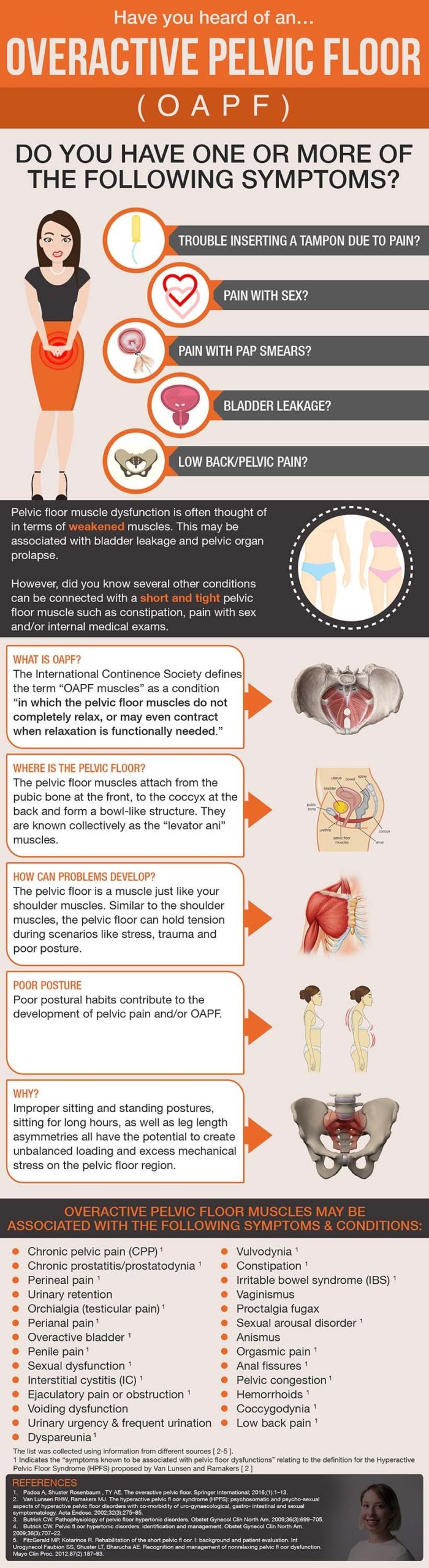
One of the reasons an overactive pelvic floor goes undiagnosed for so long is that its symptoms do not appear to belong together. An infographic produced by Inform Physiotherapy in Melbourne lists the kinds of things patients report: pain inserting a tampon, pain during sex, pain during pap smears, bladder leakage, low back or pelvic pain. Taken individually, each of those might be attributed to something else entirely. Taken together, they point towards a pelvic floor that cannot release.
The mechanics make sense once you understand that the pelvic floor is not only about holding on. It also needs to lengthen and let go for urination, bowel movements, penetration and comfortable pelvic examinations. When the muscles stay tense, pain can show up locally as vulval or pelvic discomfort, or be felt as referred pain into the hips, back or pelvis. Bladder and bowel symptoms can appear because normal emptying requires that release. Penetration can become painful or feel impossible when the muscles spasm or guard.
The Inform infographic also lists a broader set of conditions an overactive pelvic floor may be associated with, including chronic pelvic pain, IBS-related symptoms, vaginismus, and various urinary symptoms. The pattern is consistent: pelvic floor tension can sit underneath a lot of different complaints without ever being identified as the common thread.
The mechanics make sense once you understand that the pelvic floor is not only about holding on. It also needs to lengthen and let go for urination, bowel movements, penetration and comfortable pelvic examinations. When the muscles stay tense, pain can show up locally as vulval or pelvic discomfort, or be felt as referred pain into the hips, back or pelvis. Bladder and bowel symptoms can appear because normal emptying requires that release. Penetration can become painful or feel impossible when the muscles spasm or guard.
The Inform infographic also lists a broader set of conditions an overactive pelvic floor may be associated with, including chronic pelvic pain, IBS-related symptoms, vaginismus, and various urinary symptoms. The pattern is consistent: pelvic floor tension can sit underneath a lot of different complaints without ever being identified as the common thread.
Inform Physio’s Overactive Pelvic Floor Explainer
Inform Physiotherapy has produced a visual explainer covering the symptoms, associated conditions and treatment pathway for overactive pelvic floor. It is designed to be shared and is a useful starting point for anyone who recognises the symptom list but has never seen the condition named.
View the explainer: Overactive Pelvic Floor infographic

When the instinct to strengthen makes things worse
This is where the standard advice goes sideways. A person experiencing leakage or pelvic discomfort will often be told, by the internet, by friends, sometimes even by health professionals who have not assessed the pelvic floor directly, to do more strengthening exercises. For a hypertonic pelvic floor, that is like telling someone with a clenched jaw to bite harder.
The Better Health Channel notes that pelvic floor dysfunction is not only about weakness: muscles can be weak but overactive, working too hard, which can contribute to issues including painful sex, vulval pain and bladder control problems. It is a useful distinction, and one that challenges the idea that pelvic floor care is a one-size-fits-all proposition.
The first goal with an overactive pelvic floor is commonly down-training: learning how to relax, coordinate and control the muscles rather than bracing them harder. A patient information leaflet from Imperial College Healthcare NHS Trust describes the treatment approach as a pyramid, starting with education, breathing and relaxation at the base, then progressing to active relaxation and manual therapy when appropriate.
What treatment actually involves
Pelvic health physiotherapy for an overactive pelvic floor typically begins with a detailed history and symptom assessment, followed (when appropriate) by an examination to assess pelvic floor tone and control. From there, the focus shifts to relaxation and breathing strategies to reduce guarding, techniques to improve awareness and the ability to lengthen or release the pelvic floor, and a gradual return to comfortable function and movement. Lifestyle contributors like toileting habits may also be addressed.
None of this is dramatic. It is careful, structured and, for many people, revelatory. The moment someone realises they can learn to let those muscles go, after months or years of unconscious bracing, is often described as a turning point. Not because the symptoms vanish overnight, but because the problem finally has a name and a direction.

Why people live with it for so long
There are practical reasons this condition stays hidden. The symptoms sit in territory most people find difficult to discuss: pain during sex, bladder accidents, discomfort during intimate medical examinations. They accumulate in private. They get absorbed into the background noise of daily life. And the cultural default, strengthen your pelvic floor, feels so commonsense that questioning it rarely occurs to anyone.
The result is that many people spend years managing symptoms individually (a pad for leakage here, avoidance of intimacy there, a quiet dread of pap smears) without anyone connecting the dots. An assessment by a pelvic health physiotherapist can clarify whether the pelvic floor is overactive, weak, poorly coordinated, or a combination of all three, which is common.

A starting point, not an endpoint
Inform Physiotherapy in Melbourne’s Fairfield and Carlton offers pelvic health physiotherapy with experienced clinicians who assess, diagnose and treat conditions including overactive pelvic floor. Their infographic, designed to be shared and displayed in clinic waiting rooms, is doing a specific and useful job: helping people recognise that symptoms they have been dealing with alone may have a name, and that a pelvic health physiotherapist can assess what is going on and guide treatment.
If the symptom list feels uncomfortably familiar, the most useful next step is usually not guessing exercises from the internet. It is getting an assessment that establishes what the pelvic floor is actually doing, and building a plan from there.
If the symptom list feels uncomfortably familiar, the most useful next step is usually not guessing exercises from the internet. It is getting an assessment that establishes what the pelvic floor is actually doing, and building a plan from there.
How to book
| Detail | Info |
|---|---|
| Service | Pelvic Health Physiotherapy |
| Fairfield clinic | 87 Arthur Street, Fairfield 3078 |
| Carlton clinic | 54 Elgin Street, Carlton 3053 |
| Phone | 03 9481 6312 |
| Book online | informphysio.com |
The pelvic floor is a small group of muscles with an outsized influence on daily life. When it works well, nobody thinks about it. When it does not, it can quietly reshape how a person moves, sleeps, exercises, and relates to their own body. The difference between tolerating that and treating it often starts with a single question: could these muscles be doing too much, not too little?
This article is general information only and does not replace individual medical advice. If you have pelvic pain, bladder or bowel changes, or sexual pain, consult a qualified healthcare professional.